
Eligibility Verification and Prior Authorization
Eligibility and insurance verification are vital to ensuring accurate and timely receipt of information regarding insurance coverage. Without proper checks and balances in place, a healthcare organization could be leaving money on the table. Failure to confirm eligibility and achieve prior authorization can lead to delayed payments and denials, resulting in decreased collections and revenues.
Prompt and accurate determination of the patient’s eligibility on the front-end provides healthcare providers a clear view of the patient’s coverage, out-of-network benefits and payment obligation. Eligibility verification processes help healthcare providers submit clean claims. It avoids claim resubmission, reduces demographic or eligibility-related rejections and denials, increases upfront collections; leading to improved patient satisfaction and improving medical billing.
Leverage Harrington Medical Billing Services's Eligibility Verification and Prior Authorization services to optimize your revenue cycle and improve collections.
ELIGIBILITY AND BENEFITS VERIFICATION SERVICES
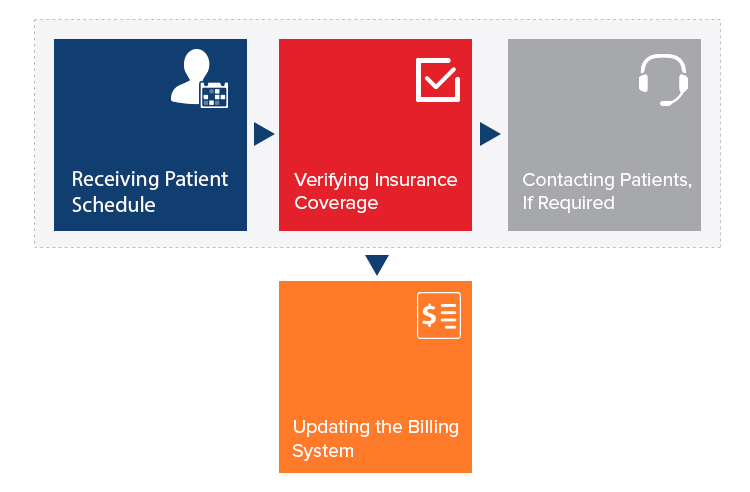
- Workflows received through the patient scheduling system, EDI, Fax, emails and FTP files
- Accurate verification of primary and secondary coverage details, including member ID, group ID, coverage period, co-pay, deductible and co-insurance and benefits information
- Efficient connection with the payer using the best possible channel (phone or web)
- Prompt identification and resolution of missing or invalid data
- Upgrade eligibility verification processes with our proprietary RPA tools
PRIOR AUTHORIZATION
- Rapid determination of prior authorization requirements
- Prepare and submit paperwork to the payer
- Consistent follow-ups on submitted prior-authorization requests
- Immediate notification of any issues with the authorization request
HARRINGTON MBS VALUE PROPOSITION FOR ELIGIBILITY VERIFICATION SERVICES
- Optimized cash flow
- Reduced patient-related denials
- Avoided rejection of claims by payers due to inaccurate or incomplete information
- Identification of the patient’s responsibility upfront
- Improved patient satisfaction